
At Khandwala’s Eye hopsital it is our endeavor to make every patient a participant in his/her treatment process.
As a part of this policy, we would like to answer some of the common queries about various eye diseases.
Cataract Surgery
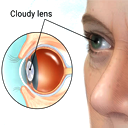
What is a Cataract Surgery ?
When the natural lens in the eye loses its transparency it prevents light from focusing clearly in the eye. This is known as Cataract.What causes Cataract ? Old age, Injury to the eye, Other factors eg. Diabetes, Myopia can speed up cataract formation.
What is the treatment?
Progress of cataract cannot be halted. Surgery is the only treatment.What type of surgery is required ?
The cataractous lens is removed by eitherConventional Method or Phacoemulsification method. In either technique an Intraocular Lens is implanted in the eye.What is Phacoemulsification?
This is the latest technology for cataract removal. The cataract is "melted" in the eye and "sucked" out through a very small wound with the help of a special probe.How safe is Phacoemulsification?
This is a safe & most preferred technique of cataract removal the world over.When can Phacoemulsification be performed?
It is not necessary to wait for the cataract to,"mature" Phacoemulsification cataract surgery can be performed at any time.What are the different types of Intraocular Lens?
There are 2 types of IOLS. A) Hard Lenses (RIGID) / Conventional | Large wound required for implantation, B) Soft Lenses Foldable/Injectable), Latest type of lenses | Very small wound is required | Biocompatible material.Note :
Lasik Surgery
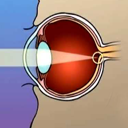
What is a Lasik Surgery ?
Lasik stands for laser in Situ Keratomileusis. It is a form of laser surgery that is capable of correcting nearsightedness, farsightedness and astigmatism. The procedure uses a Computer controlled Excimer Laser to reshape the cornea to correct the vision. The laser reshaping is done under a protective flap of tissue to promote a very rapid recovery of vision and minimize discomfort.What are the criteria for patient selection in LASIK surgery?
Patient should be above 18 years of age & Have stable refraction for 6 months.Up to what power of refractive error (glasses number) can be corrected by LASIK ?
Lasik surgery can correct : Myopia from -1.00 to -12.00D | Hypermetropia from +1.00 to +6.00D | Astigmatism from -1.00 to -6.00D & +1.00 to +6.00D.How long does the procedure take ?
The LASIK procedure takes about 10 minutes per eye.Is the surgery procedure painful?
No! Anaesthetic drops usually allow the operation to be performed without pain.What are the restrictions following surgery?
The usual restrictions after surgery are that a protective shield should be worn to bed for the first week. Swimming is not advisable for one week after surgery, although bathing and showering is fine. No eye make up should be applied for 7 days. All other activities may be resumed on the first day following surgery. The procedure can be performed on both eyes at once if required. Most patients choose this option as it is far more convenient.Are glasses required even after the procedure ?
This will depend on a number of factors, including the refractive error, the visual needs, and even your personality. It is important to understand that LASIK does not eliminate the need for reading glasses as one grows older.What are the usual side effects?
The patient's vision will fluctuate during the few days following surgery. The patient may notice some glare around lights at night. There may be a feeling of dryness in the eyes. Rarely a patient may have persistence of one or more of these effects. These effects are usually more during the first two weeks after surgery and then slowly disappear.What are the complications of the surgery ?
Like any surgical procedure, LASIK carries some risk of complications, although they are not vision threatening, The patient get back to work usually after 3 days of the surgery.Diabetic Retinopathy
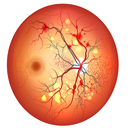
Diabetic Retinopathy ?
Diabetic retinopathy (die-uh-BET-ik ret-ih-NOP-uh-thee) is a diabetes complication that affects eyes. It's caused by damage to the blood vessels of the light-sensitive tissue at the back of the eye (retina). At first, diabetic retinopathy may cause no symptoms or only mild vision problems.Who's at the most risk for diabetic retinopathy ?
Fluctuating blood sugar levels increase risk for this disease, as does long-term diabetes.Most people don't develop diabetic retinopathy until they've had diabetes for at least 10 years. However, adult onset (type 2) diabetics should be evaluated at the time of diagnosis and every year thereafter, whereas juvenile onset (type 1) diabetics should be evaluated five years after diagnosis and every year thereafter, at a minimum.Is there any way to prevent diabetic retinopathy?
Keeping your blood sugar at an even level can help prevent diabetic retinopathy. If you have high blood pressure, keeping that under control is helpful as well. Even controlled diabetes can lead to diabetic retinopathy, so you should have your eyes examined once a year; that way, your doctor can begin treating any retinal damage as soon as possible.What are the signs and symptoms of diabetic retinopathy ?
In the early stages of diabetic retinopathy, you might have no symptoms at all, or you might have blurred vision. In the later stages, you may develop cloudy vision, blind spots or floaters. But never assume that good vision means all is well in the retina! This can be a setup for disaster.What are the different types of diabetic retinopathy ?
Diabetic retinopathy is classified as either nonproliferative (background) or proliferative. Nonproliferative retinopathy is the early stage, where small retinal blood vessels break and leak. In proliferative retinopathy, new blood vessels grow abnormally within the retina. This new growth can cause scarring or a retinal detachment, which can lead to vision loss. The new blood vessels may also grow or bleed into the vitreous humor, the transparent gel filling the back of the eye in front of the retina. Proliferative retinopathy is much more serious than the nonproliferative form and can lead to total blindness.Is Diabetic Retinopathy Curable ?
No. Early treatment can slow the progression of diabetic retinopathy, but is not likely to reverse any vision loss.What diabetic retinopathy treatments are currently available ?
The best treatment is to keep your diabetes under control; blood pressure control also helps.Your doctor may decide on laser photocoagulation to cause regression of leaking blood vessels and prevent new blood vessel growth. If blood gets into the vitreous humor, your doctor might want to perform a procedure called a vitrectomy.Also, there are a number of new diabetic retinopathy treatment options currently in clinical trials or other stages of development.Age Related Macular

What is Age Related Macular ?
Age Related Macular Degeneration (AMD) is a disease associated with aging, characterized by damage to the central part of the retina called macula.Dry AMD & Wet AMD ?
Dry AMD is the most common form found in 90% of patients. Dry AMD occurs when the macular tissues get thin and slowly lose function. The most common symptom of dry AMD is blurred vision which causes difficulty in recognizing faces, increases light requirement for reading and other tasks. Visual deterioration is slow but usually not profound. About 10-20% of people with dry AMD advance to the wet form. Wet AMD is the less common but more aggressive form of AMD. If it is not treated it may get worse rapidly. Wet AMD is caused by proliferation of abnormal blood vessels under the retina which may exude or leak out fluid, or bleed and ultimately lead to the formation of a scar under the retina.Symptoms of AMD ?
Diminution of vision in an important symptom of macular degeneration. This lack of ability to see objects clearly affects ones ability to read, drive and see details.Straight lines appear crooked or wavy , A dark area appears in the centre of vision e.g. words in the central part of the page look smudged. Having one or more of these symptoms may not necessarily mean that one has AMD and it warrants an immediate eye check up (early detection is important).Risk Factors for AMD ?
Age - is the greatest risk factor. Although AMD can occur during middle age, studies show that people over 60 years of age are at great risk. The risk increases with increasing age. Family History of AMD increases the risk. Race - White populations are more predisposed to suffer vision loss from neovascular AMD than Asian or African populations. Smoking has a definite correlation. History of hypertension, heart disease, or lung infection adds to risk.Detection of AMD ?
Early detection is important as smaller lesions have a better recovery and chance of maintaining reading vision than advanced cases with larger lesions and fibrotic changes. Your ophthalmologist may suspect AMD if you are over 60 years of age and have recent changes in central vision. To establish a diagnosis a comprehensive eye check up is done.Macular Degeneration

What is Macular Degeneration ?
Macular Degeneration is considered an incurable eye disease.Macular Degeneration is caused by the deterioration of the central portion of the retina, the inside back layer of the eye that records the images we see and sends them via the optic nerve from the eye to the brain. The retina’s central portion, known as the macula, is responsible for focusing central vision in the eye, and it controls our ability to read, drive a car, recognize faces or colors, and see objects in fine detail.One can compare the human eye to a camera. The macula is the central and most sensitive area of the so-called film. When it is working properly, the macula collects highly detailed images at the center of the field of vision and sends them up the optic nerve to the brain, which interprets them as sight. When the cells of the macula deteriorate, images are not received correctly. In early stages, macular degeneration does not affect vision. Later, if the disease progresses, people experience wavy or blurred vision, and, if the condition continues to worsen, central vision may be completely lost. People with very advanced macular degeneration are considered legally blind. Even so, because the rest of the retina is still working, they retain their peripheral vision, which is not as clear as central vision.Risk Factors ?
The biggest risk factor for Macular Degeneration is age. Your risk increases as you age, and the disease is most likely to occur in those 55 and older. Other risk factors include: Genetics – People with a family history of MD are at a higher risk. Smoking – Smoking doubles the risk of macular degeneration.Are there any Treatment ?
There is currently no known cure for Macular Degeneration, but there are things you can do to reduce your risk and possibly slow the progression once you’ve been diagnosed. For example, one can pursue lifestyle changes like dieting, exercise, avoiding smoking, and protecting your eyes from ultraviolet light.Dry Eyes
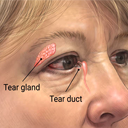
What is Dry Eyes ?
When you blink, a film of tears spreads over the eye, making the surface of the eye smooth and clear. Without this tear film, good vision would not be possible.Sometimes people don't produce enough tears or the right quality of tears to keep their eyes healthy and comfortable. This condition is known as dry eye.Causes of Dry Eye ?
Hormonal changes are a main cause of dry eye syndrome, causing changes in tear production. The hormonal changes associated with menopause are one of the main reasons why women are most often affected by dry eye.Conditions that affect the lacrimal gland or its ducts — including autoimmune diseases like lupus and rheumatoid arthritis — lead to decreased tear secretion and dry eye. Tear secretion also may be reduced by certain conditions that decrease corneal sensation. Diseases such as diabetes and herpes zoster are associated with decreased corneal sensation. So is long-term contact lens wear and surgery that involves making incisions in or removing tissue from the cornea (such as LASIK).Another cause for dry eye is exposure to a dry, windy climate, as well as smoke and air conditioning, which can speed tear evaporation. Avoiding these irritants can offer dry eye relief.Dry Eye Symptoms ?
While it may sound strange, people with dry eye may find their eyes water quite a bit. This is because the eye is responding to the irritation of this condition. Dry-eye sufferers may find that they feel like they cannot keep their eyes open for very long. They may also find their eyes feel more uncomfortable after reading or watching television. Dry eye symptoms usually include:Stinging or burning eyes; Scratchiness; Stringy mucus in or around the eyes; Excessive eye irritation from smoke or wind;Excess tearing; Discomfort when wearing contact lenses.Dry Eye Treatments..
Preservative-free eyedrops are available for people who are sensitive to the preservatives in artificial tears. If you need to use artificial tears more than six times a day, preservative-free brands may be better for you.You can use the preservative-free artificial tears as often as necessary — once or twice a day or as often as several times an hour.Conserving your eyes' own tears is another approach to keeping the eyes moist. Tears drain out of the eye through a small channel into the nose (which is why your nose runs when you cry). Your ophthalmologist may close these channels either temporarily or permanently. This method conserves your own tears and makes artificial tears last longer. Other methods : Tears evaporate like any other liquid. You can take steps to prevent evaporation. In winter, when indoor heating is in use, a humidifier or a pan of water on the radiator adds moisture to dry air. Wraparound glasses may reduce the drying effect of the wind.A person with dry eye should avoid anything that may cause dryness, such as an overly warm room, hair dryers or wind. Smoking is especially bothersome.Some people may find dry-eye relief by supplementing their diet with omega-3 fatty acids, which are found naturally in foods like oily fish (salmon, sardines, anchovies) and flax seeds. Ask your Eye M.D. if you should take supplements of omega-3 fatty acids and, if so, in what form and dosage. If you are bothered by dry eye, talk with your Eye M.D. for ways to find relief.Contact Lenses

